Let's cut to the chase. Pregnancy isn't a time to play guessing games with medications. Up to 90% of pregnant women use at least one medication, and figuring out what's safe can feel like navigating a minefield. I've spent over a decade counseling expectant mothers, and the confusion is real—but it doesn't have to be. This guide breaks down exactly what medications are used in pregnancy, what to avoid, and how to work with your doctor without the panic.
Quick Navigation: Jump to What Matters
Why Medication Use in Pregnancy Isn't Black and White
Here's something many websites gloss over: avoiding all medications during pregnancy isn't always the safest choice. Think about it. If you have a urinary tract infection, leaving it untreated can lead to kidney issues or preterm labor. The key is balancing risks. The U.S. Food and Drug Administration (FDA) used a pregnancy category system (A, B, C, D, X), but they've moved to a more detailed labeling approach. Still, old habits die hard, and many doctors reference those categories.
From my experience, one common mistake is assuming "natural" equals safe. Herbal supplements like echinacea or high-dose vitamin A can pose risks. Always check with a healthcare provider—don't rely on internet forums.
Medications are often needed for chronic conditions like asthma, depression, or thyroid disorders. Stopping them abruptly can harm both mother and baby. A study from the Centers for Disease Control and Prevention (CDC) highlights that managing pre-existing conditions is crucial for healthy outcomes.
Common Pregnancy-Safe Medications: A Detailed Look
Let's get specific. Below is a table summarizing key medication categories, but remember, dosage and timing matter. Always consult your doctor before taking anything.
| Medication Category | Common Examples | Safety Notes (Based on FDA Data) | Typical Uses |
|---|---|---|---|
| Pain and Fever Relievers | Acetaminophen (Tylenol) | Generally considered safe when used as directed. Avoid high doses. | Headaches, muscle aches, fever |
| Ibuprofen (Advil) or Naproxen | Avoid especially in third trimester; may cause complications. | Inflammation, pain (use with caution) | |
| Antibiotics | Penicillins (e.g., Amoxicillin), Cephalosporins | Often safe for bacterial infections like UTIs or strep throat. | Infections |
| Avoid Tetracyclines | Can affect fetal bone and teeth development. | Not recommended | |
| Allergy and Cold Meds | Loratadine (Claritin), Cetirizine (Zyrtec) | Generally safe; prefer second-generation antihistamines. | Allergies, runny nose |
| Pseudoephedrine (Sudafed) | Use with caution; avoid in first trimester due to potential risks. | Congestion | |
| Gastrointestinal Issues | Antacids (e.g., Tums), Metoclopramide (Reglan) | Often safe for heartburn or nausea. | Digestive discomfort |
| Chronic Conditions | Levothyroxine (thyroid), Insulin (diabetes) | Essential for managing conditions; stopping can be dangerous. | Thyroid disorders, diabetes |
Now, let's dive deeper. For pain, acetaminophen is the go-to, but I've seen women overuse it thinking it's harmless. Stick to the recommended dose—no more than 3,000 mg per day. For antibiotics, penicillins are usually fine, but always finish the course to prevent resistance.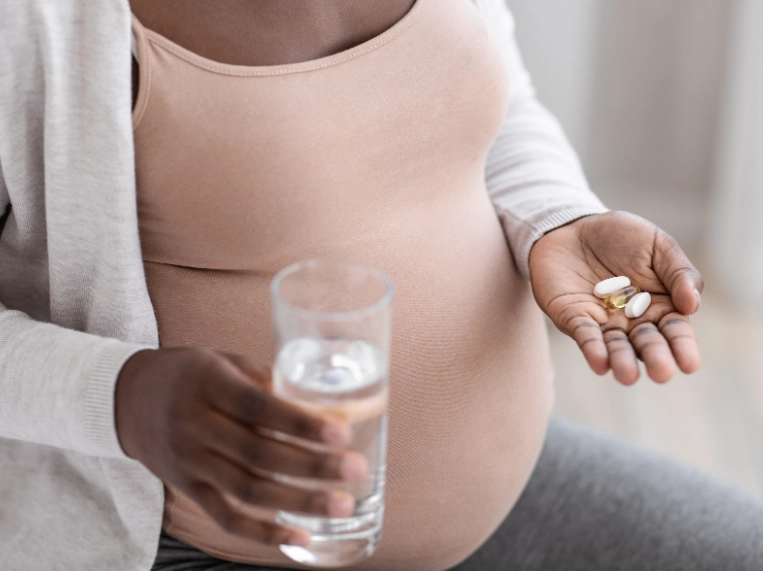
For Morning Sickness: What Actually Works
Morning sickness can be brutal. Over-the-counter options like vitamin B6 and doxylamine (found in some sleep aids) are often recommended. Prescription drugs like ondansetron (Zofran) are used for severe cases, but discuss risks with your doctor. A non-medication tip? Try ginger tea or small, frequent meals.
Mental Health Medications: A Delicate Balance
This is where things get tricky. SSRIs like sertraline (Zoloft) are commonly used for depression during pregnancy. The risk of untreated depression—like poor prenatal care—often outweighs medication risks. I recall a patient who stopped her antidepressants cold turkey and struggled with severe anxiety. Work with a psychiatrist who specializes in perinatal care.
Red Flags: Medications to Steer Clear Of
Some drugs are a hard no. Here's a quick list:
- Isotretinoin (Accutane): Used for acne, it's known to cause severe birth defects. Absolute avoidance is key.
- Warfarin (Coumadin): A blood thinner that can harm fetal development; alternatives like heparin are safer.
- ACE Inhibitors (e.g., Lisinopril): For high blood pressure, but avoid during pregnancy due to kidney risks for the baby.
- Certain Anticonvulsants: Like valproic acid, linked to neural tube defects.
Don't forget over-the-counter stuff. Avoid high-dose aspirin unless prescribed—it can increase bleeding risks. And skip herbal remedies like black cohosh, which might induce labor prematurely.
One subtle error? Assuming all topical medications are safe. Retinoids in skincare creams can be absorbed and pose risks. Check labels.
How to Discuss Medications with Your Doctor: A Step-by-Step Guide
Talking to your doctor shouldn't be intimidating. Here's a practical approach:
Step 1: Make a list. Write down all medications you're taking—prescription, over-the-counter, supplements. Include dosages.
Step 2: Ask specific questions. Instead of "Is this safe?" try "What are the known risks for this drug in the second trimester?" or "Are there alternatives with less fetal exposure?"
Step 3: Discuss timing. Some medications are safer in certain trimesters. For example, ibuprofen might be okay early on but not later.
Step 4: Get a second opinion if needed. If your doctor dismisses your concerns, consult a maternal-fetal medicine specialist. I've seen cases where a quick switch to a safer drug made all the difference.
Step 5: Monitor together. Keep a log of any side effects and report them. Your doctor can adjust as needed.
Remember, you're a team. Bring a partner or notes to appointments—pregnancy brain is real, and details matter.
Your Burning Questions on Pregnancy Medications Answered
Wrapping up, medications during pregnancy require a careful, informed approach. Don't rely on hearsay—use this guide as a starting point and partner with your healthcare team. Every pregnancy is unique, and what works for one person might not for another. Stay proactive, ask questions, and prioritize both your health and your baby's well-being.
Reader Comments